Thursday, 28th August 2025.

by inAfrika Reporter
African health agencies have launched a continent-wide cholera response plan amid a deadly surge in Sudan and persistent outbreaks across multiple countries. The initiative, discussed this week alongside World Health Organization (WHO) partners, targets a 90% reduction in cholera deaths and elimination in more than 20 countries by 2030, with an initial funding call of about $231 million for rapid actions over the coming months. Officials say the plan prioritizes clean water and sanitation investments, faster diagnostics and case management, and the strategic deployment of limited oral cholera vaccine (OCV) supplies.
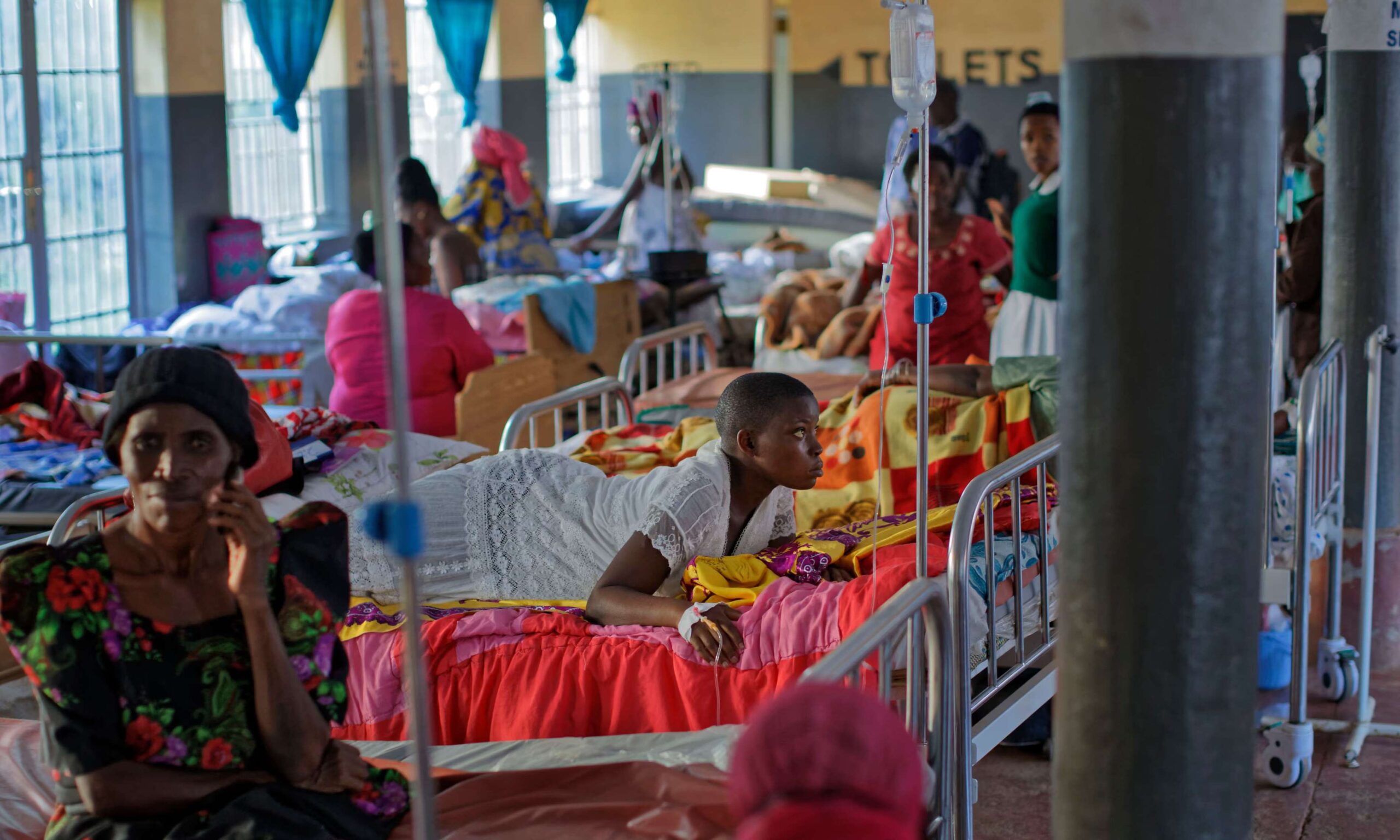
The urgency is clearest in Sudan, where war and mass displacement have driven the disease into nearly all states. WHO’s regional office reports that cholera has spread widely amid collapsing health services and the rainy season, compounding the risks of famine and water-borne diseases. Aid groups and authorities have rolled out vaccination campaigns in hotspots like Khartoum and Darfur, but access and security constraints have slowed delivery. Recent updates underline the scale: roughly 100,000 suspected cases and more than 2,400 deaths since last year, with spikes in weekly fatalities as treatment centers are overwhelmed.
Beyond Sudan, cholera remains entrenched across parts of central, eastern, and southern Africa. ReliefWeb summaries drawing on Africa CDC and national ministries highlight new waves in countries like Chad and the Democratic Republic of Congo (DRC), where case counts reached tens of thousands this year. The disease exploits weak water, sanitation, and hygiene (WASH) systems—especially in displacement camps, flood-affected areas, and informal urban settlements. That’s why the continental plan couples emergency response with structural fixes: expanding safe water access, rehabilitating boreholes, and financing climate-resilient sanitation to blunt the cycle of outbreak, response, and relapse.
A persistent constraint is vaccines. Global OCV supplies are stretched, forcing rationing strategies, single-dose campaigns, and tough prioritization. Health officials emphasize that vaccines are only one layer; without sustained WASH investment, cholera will keep returning. Still, targeted use of OCV—combined with rapid rehydration therapy, antibiotics in severe cases, and public awareness on safe water—can sharply reduce deaths even in fragile settings. The plan aims to pre-position cholera kits, expand lab capacity, and standardize surveillance so authorities can detect clusters earlier and move faster.
The politics of funding will determine success. Africa CDC’s weekly briefings throughout July flagged “increasing cholera outbreaks in several Member States,” tying spikes to extreme weather and strained public systems. Donors are being asked to move beyond one-off grants to multi-year packages that link humanitarian response with development finance—so rebuilt water systems don’t collapse once emergencies fade from headlines. The strategy also leans on domestic resource mobilization, arguing that preventing outbreaks is cheaper than repeatedly fighting them.
For East Africa, the stakes are immediate. Outbreaks have hit countries from Ethiopia and Kenya to Tanzania and Uganda in recent seasons, often following floods or in dense border towns where cross-border movement is essential for trade. Coordinated surveillance—sharing alerts across borders and harmonizing case definitions—could stop localized flare-ups from exploding into regional crises. Authorities are also working with schools and local media on handwashing and water treatment messaging to keep fatality rates low when cases rise.
Can the plan work? Evidence says yes—if funding lands quickly and WASH is prioritized alongside vaccines. Countries that invested in chlorination points, rapid diagnostic tests, and community health workers have cut fatality rates below 1% even during large waves. But with conflict, climate shocks, and urbanization accelerating, the window for prevention narrows without sustained financing. The $231 million ask is a starting point, not an endpoint.
For readers in Tanzania and the wider region, the takeaway is practical: boil or treat water, wash hands frequently, and seek care fast for severe diarrhea—especially for children. At the policy level, track how much of the pledged cholera money goes into permanent water and sanitation upgrades. That’s what turns a short-term plan into lasting resilience